We Keep Healthcare Healthy™
We make DME rental simple and oxygen management easy.
DME Rentals →
Oxygen Tank Program →
We Keep Healthcare Healthy™
We make DME rental simple and oxygen management easy.
DME Rentals →
Oxygen Tank Program →

DME Rentals and Oxygen Tank Program
Medical Oxygen Therapy →
Respiratory Therapy →
Durable Medical Equipment →
Same-day Response. 24/7 Emergency Availability.
Same-day Delivery. Guaranteed.
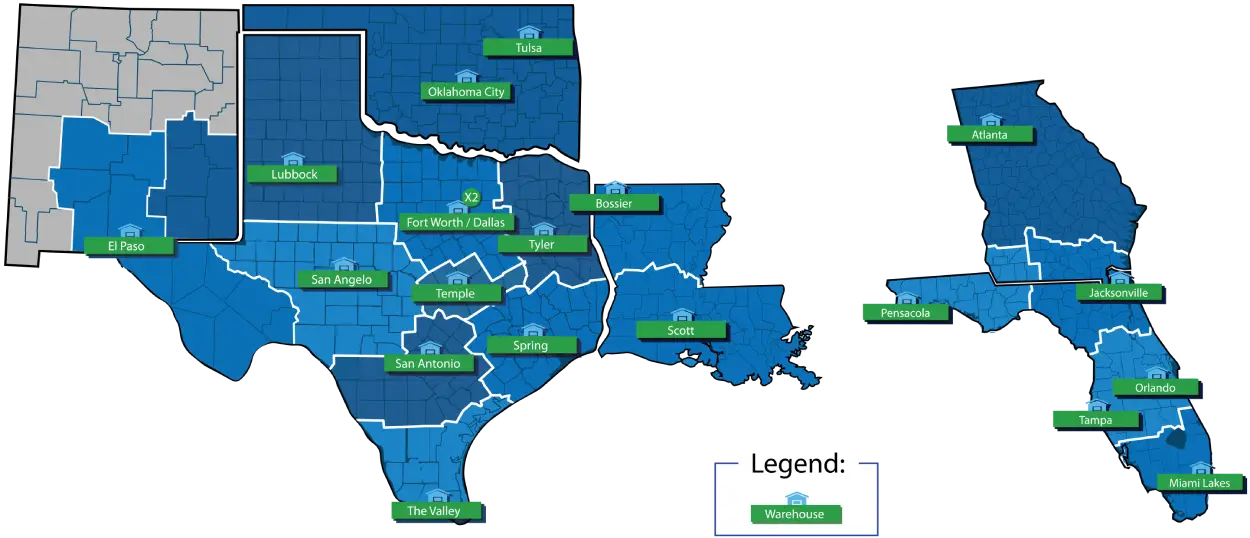

Your Single Source for Same-day DME Delivery and Better Facility Hygiene


Online Equipment Portal
As a service to our customers, our Online Equipment Portal makes real-time equipment management easier, convenient, and better. It becomes your one-stop shop dashboard to get proactive insights and services right from your desktop 24/7. Our partners with multiple facilities can access all the information needed for each facility in a single, compiled, and online location. Our portal places all necessary information at the touch of your fingers. The real-time interface complies with all billing, rentals, requests, and more in a single, easily accessible location.
Easy Connect
Better Operational Efficiency
Improves Your Financial Performance
The Difference You Will Experience
Reliable
Our guaranteed same-day delivery, rigorous equipment and product evaluations, and leading infection prevention protocols ensure you will receive the best equipment at the right time.
Transparent
Our quarterly business reviews (QBRs) and online equipment portal ensure you are never in the dark with your spend and utilization.
Consistent
Never worry if your medical equipment or facility hygiene provider will show up when you need them the most. We ensure all customers are fully equipped to treat their residents and support their staff-especially in emergencies.
Effective
We supply you with best-in-class equipment and industry-leading facility hygiene products. As a OneSource provider you will always have the products you need when you need it the most.

-Gary Blake, CEO, Creative Solutions in Healthcare



